Discussion
The first main objective of this study was to examine whether perceived levels of job stress, burnout, and mental health of medical faculty members were different according to demographic characteristics and working conditions.
First, demographic characteristics made significant group differences in perceived levels of job stress, burnout, and mental health of medical faculty members. Women perceived higher stress from daily tasks, burnout in emotional exhaustion and depersonalization, and depression and retirement at medical schools than men. The finding is similar to other studies where female doctors showed higher occupational stress and burnout levels than males [
4,
12,
17]. Cassidy-Vu et al. [
18] articulated that higher levels of burnout among female faculty members are often attributable to gender-specific difficulties in clinical expectations and maintenance of work-life balance.
Age increase reversely decreased the risk of burnout and adverse mental health among medical faculty members, i.e., the highest for those aged 30s and the lowest for those aged 60 years old and more, which were similar to the findings of other studies [
3,
17]. Marital status made a group difference only in emotional exhaustion, similar to another study [
4].
Medical faculty members whose institutions locate in Chungcheong area and Gyeongsang area showed the highest or the second highest levels of three job stressors, burnout in emotional exhaustion and depersonalization, and depression and retirement. The specialties of the faculty members at the institutions might cause this kind of regional difference, which was not evenly distributed over the country. Further studies need to scrutinize factors related to regional difference.
Second, working conditions significantly differentiated the levels of job stress, burnout, and mental health of medical faculty members. Medical faculty members working at both hospitals and schools showed the highest levels for all three stressors, depression, and retirement. Meanwhile, those working at the hospital only experienced the highest burnout in emotional exhaustion and depersonalization. Physicians taking care of critically ill patients at hospitals can disclose higher stress levels than those working at universities and research institutes.
Associate professors and assistant professors responded with the highest and the second highest levels of job stress, burnout, and adverse mental health compared to professors or clinical professors, who are usually overwhelmed with several duties of clinical care, education, and research simultaneously to achieve performance and promotion at the institutions. Those employed 10–14 years showed the highest stress level for daily tasks. Academic rank and employment period have a positive correlation (r=0.699, p<0.01), with the professors employed 15 years or more showing the lowest stress level for daily tasks. Those working 52–79 hours a week showed the highest stress level in the daily tasks and the highest burnout level in personal accomplishment, closely related to heavy workloads during regular working hours [
17,
19].
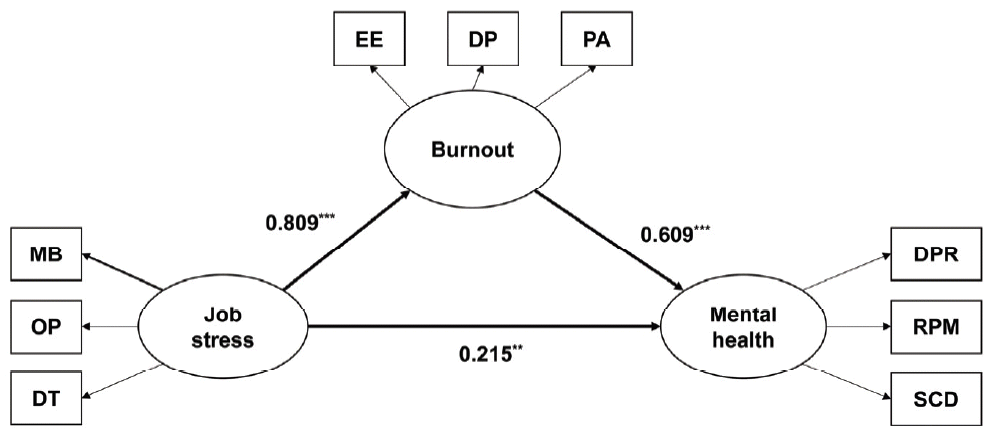
Third, this study found direct and indirect effects of job stress on the mental health of medical faculty members, with the indirect effect bigger than the direct effect and the mediating effect of burnout between the two variables as hypothesized. The findings in this study support several prior studies where job stress affect burnout [
3-
8], job stress and burnout affect mental health [
1,
10,
11,
13,
14]. Further, this study could construct a causality among these three latent variables, i.e., job stress, burnout, and mental health.
It is essential to identify the mediating effect of burnout, as it is possible to intervene not only in job stress but also in burnout to prevent the adverse mental health of medical faculty members. Therefore, it needs prevention strategies to minimize burnout as well as job stress, such as proper work schedule, reduced workloads, recruitment of more faculty members and at institutional and organizational levels, regular exercise, counseling and psychological health services, and social support at the individual level [
4,
6,
20]. Medical faculty members should take active and adaptive coping skills to reduce burnout and should avoid maladaptive coping strategies such as self-blame and denial [
11].
Our study has several limitations to be mentioned for future studies. First, this study missed very crucial variables such as work intensity, specialty, night shifts, on calls, patient volume, frequency of treatment, and so forth, which were found to be significantly associated with job stress, burnout, as well as mental health of medical school personnel in other studies [
3,
4,
6,
8,
17]. Researchers should include these variables for future studies and consider how to measure these variables to input structured causal relationships. Second, no responses from some medical faculty members may threaten the generalization of the results, even though this study used a nationwide data set for the analyses. Third, this study measured job stress, burnout, and mental health as the perceived levels, when the respondents may not have the symptoms at the point of the survey but may develop later and vice versa as the perception is a continual state. Despite these limitations, the study findings provide concrete and comprehensive information on the perceived levels of job stress, burnout, and mental health of medical faculty members and their causal relationship, resulted with a large sample.
In conclusion, this study found that job stress has direct and indirect effects on the mental health of medical faculty members, and burnout partially mediated this relationship. Further studies need to intervene in job stress and burnout to prevent the adverse mental health of medical faculty members and to introduce proper measures to improve working conditions affecting job stress and burnout.